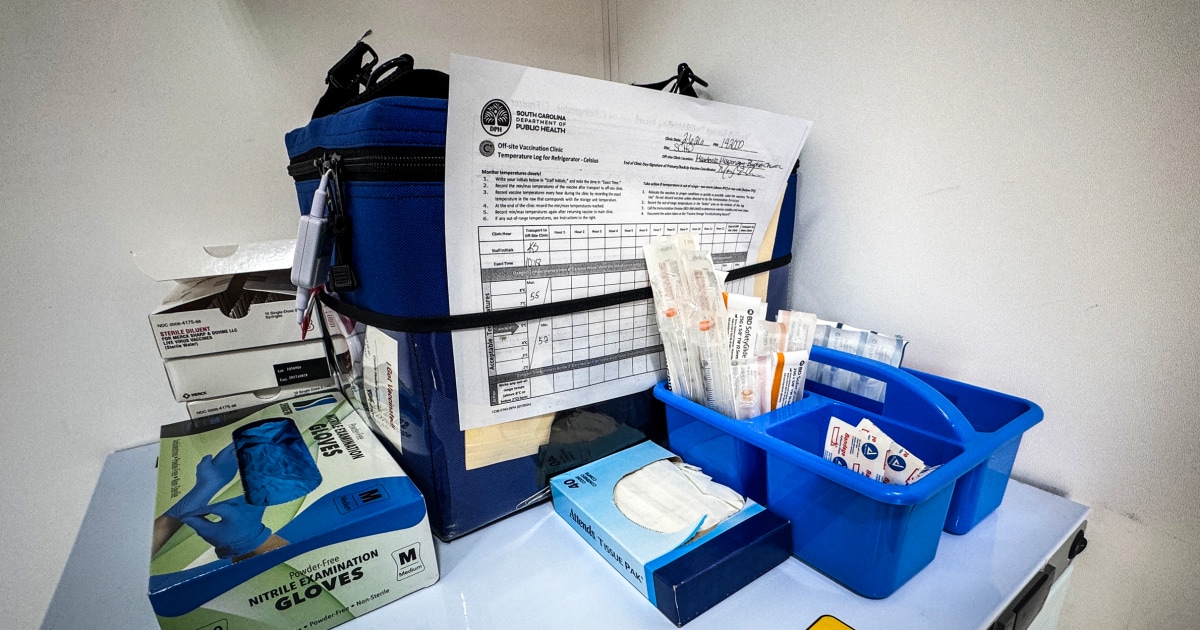
As measles outbreaks spread across the U.S., public health departments face significant financial and staffing challenges, often requesting aid that goes unanswered. A new report estimates that a 1% annual decline in measles vaccination rates could cost the nation $1.5 billion annually due to increased cases, hospitalizations, and lost productivity. The initial cost of containing an outbreak can reach hundreds of thousands of dollars, with each additional case averaging $16,000 for medical expenses and contact tracing. These economic burdens, coupled with the immeasurable human suffering from preventable disease, highlight the critical need for robust public health responses and sustained vaccination efforts.
Read the original article here
Measles outbreaks are costing the U.S. millions of dollars, but the true losses are immeasurable, a stark reality that underscores a profound societal disconnect from scientific understanding and public health.
When rational thought is seemingly abandoned, and scientific data is disregarded in favor of unsubstantiated beliefs, the consequences become alarmingly clear, as seen with resurgent measles outbreaks. The presence of individuals in positions of authority who actively promote skepticism towards established medical science, particularly concerning vaccines, exacerbates these crises. This creates a deeply concerning irony, where the very people appointed to safeguard public health are those whose viewpoints have contributed to the erosion of trust in crucial preventive measures.
The inability of some communities to grasp the severity of measles outbreaks, even when faced with active and uncontrolled spread, is a troubling symptom of this disconnect. This lack of comprehension means that reasoned arguments and clear scientific evidence often fall on deaf ears, leaving public health officials struggling to implement effective containment strategies.
Perhaps a drastic measure, though ethically complex, would be for individuals who refuse vaccination for non-medical reasons to sign waivers acknowledging they would forgo medical assistance during an outbreak, effectively choosing to bear the full consequences of their decision. This, however, doesn’t address the broader societal cost and the ripple effects of such choices.
The economic burden alone, measured in millions for healthcare maintenance and outbreak response, is significant. Yet, this pales in comparison to the potential for billions in costs if overwhelmed medical facilities become commonplace. It’s a stark reminder that preventive care, like vaccination, is an investment that saves far more than it costs.
The idea of advocating for anti-antibiotic sentiment among vaccine refusers, to highlight the perceived irrationality, points to the deeper issue of a rejection of scientific principles. If people dismiss the efficacy of antibiotics, a cornerstone of modern medicine, it logically follows that their skepticism can extend to vaccines, another critical public health tool.
The true, immeasurable losses extend far beyond financial figures, encompassing the profound suffering, lasting disabilities, and, tragically, the deaths of children who could have been protected. This tragedy is a direct consequence of a widespread distrust in science, leaving communities vulnerable and entire populations at risk. The current situation mirrors past public health crises, where the focus on monetary costs can overshadow the human toll, an approach that seemingly resonates with those in power but offers little solace to those affected.
Measles is not the only disease experiencing a resurgence, but its rapid spread highlights the vulnerability of communities with low vaccination rates. The appointment of individuals with a history of vaccine skepticism to critical health leadership roles only serves to validate these dangerous beliefs and further undermine public health efforts.
The notion of public health being politicized is a deeply concerning development that erodes critical thinking. When scientific consensus is replaced by ideological pronouncements, and education systems fail to foster robust critical thinking skills, the populace becomes more susceptible to misinformation and dangerous ideologies, including the rejection of life-saving medical interventions.
The simple, scientifically validated solution of vaccination is often sidelined in favor of irrational opposition. The suffering, disability, and potential death of children from a preventable disease should be a source of national outrage. The fact that this often fails to ignite widespread public anger, akin to the societal acceptance of other preventable tragedies, is a testament to a concerning apathy towards public health.
There’s a growing sentiment that communities actively choosing to reject protective measures should bear the direct costs of their decisions, perhaps through dedicated facilities for treatment, rather than drawing on general public funds. This perspective stems from a frustration with the perceived imposition of risk on the wider community by those who refuse to participate in collective safety measures.
The origins of these outbreaks often trace back to specific communities, some with deeply ingrained beliefs that lead them to reject scientific advice. This raises questions about why the broader society should bear the burden of outbreaks stemming from such choices, especially when the individuals making these choices express a desire to avoid interventions.
The concept of “absolute immunity” for decision-makers who disregard expert advice, leading to widespread suffering, is a dangerous loophole that undermines accountability and the rule of law. It allows for immense harm to be inflicted without consequence, eroding trust in institutions and the very fabric of a just society.
The idea of holding parents accountable for preventable child deaths, similar to how criminal negligence is treated, presents a complex legal and ethical challenge. The current societal landscape seems to navigate a precarious balance between personal autonomy and collective responsibility, often with devastating consequences for the most vulnerable.
The proposition of encouraging anti-vaxxers to also reject antibiotics, framing it as a matter of consistency in their rejection of medical science, is a satirical jab at the illogic. It highlights the selective application of skepticism and the disregard for established scientific principles, suggesting that if evolution isn’t real, then perhaps antibiotic resistance also isn’t a concern for them.
While some strategies aim to engage with skeptics by framing public health issues in economic terms, appealing to their supposed pragmatism, there’s a pessimistic outlook on its effectiveness. The disconnect between claiming to be “hard-headed pragmatists” and actual behavior suggests that these appeals may fall flat, as the underlying drivers of their beliefs are often ideological rather than rational.
A functional public health agency, like the CDC, should be actively addressing these issues, focusing on the contagious nature of diseases like measles and the critical importance of vaccination. The rapid spread of measles once vaccination rates decline underscores its contagiousness and the need for robust herd immunity.
The appointment of individuals with anti-vaccine ideologies to public health positions is a direct impediment to effective outbreak control. Their influence can validate existing skepticism and create further obstacles to vaccination campaigns.
The argument that communities that actively reject vaccines should be left to face the consequences, while controversial, stems from a deep frustration. This perspective argues that empathy should be directed towards the innocent victims – the children and vulnerable individuals who have no choice in their exposure to preventable diseases.
The contagiousness of measles is a critical factor; for every infected person, many others are at risk, making widespread vaccination the only effective shield. The validation of anti-vaccine sentiments by those in power actively undermines this defense mechanism, creating a breeding ground for outbreaks.
The notion of accountability for those who mislead the public about critical health issues is a persistent call. The deliberate dissemination of misinformation that leads to illness, suffering, and death is a grave concern that demands serious consideration.
The question of why valuable public funds are being expended to combat preventable diseases, rather than focusing on true public health crises, arises from a sense of frustration. The current approach seems to be a reactive measure to problems that could have been averted with proactive public health strategies.
The suggestion that communities choosing to forgo vaccination should be allowed to face the natural course of the epidemic, while harsh, reflects a sentiment that the societal burden of their choices should not be borne by others. This perspective is rooted in a desire to protect those who cannot protect themselves and to hold accountable those who actively undermine collective safety.
The deeply ingrained nature of certain religious or cultural beliefs that lead to the rejection of medical science, particularly vaccination, presents a significant challenge. When faith supersedes scientific understanding, it creates a barrier to public health efforts.
The argument that focusing solely on the financial cost of measles outbreaks is disheartening is a valid one. While the economic impact is substantial, it pales in comparison to the human suffering, disability, and loss of life. These are the true, unquantifiable losses that should drive public health policy.
The empathy extended to those who actively endanger others is a complex issue. Many feel that their empathy has been depleted by years of witnessing the consequences of anti-science ideologies, and that true empathy should be reserved for the victims, not the perpetrators of harm. Enabling harmful behavior, even through misguided compassion, can be seen as a form of abuse in itself.