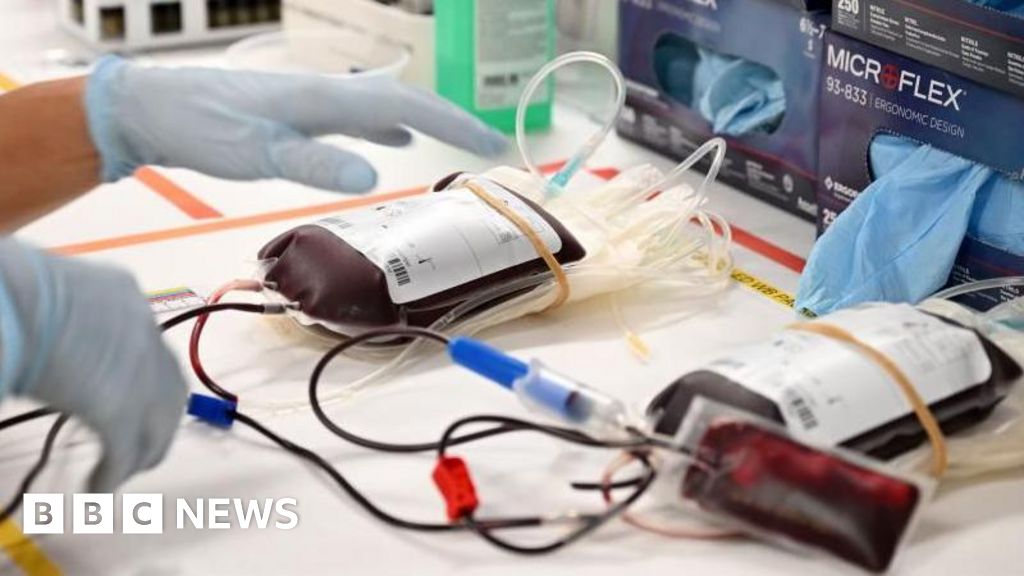
Despite a 14-year-old girl’s stated refusal of a blood transfusion due to religious convictions, legal representatives for a Scottish health board pursued an order to permit the procedure if her life was in danger. This action highlights the complex intersection of medical necessity, patient autonomy, and religious freedom, particularly when minors are involved. The case raised significant ethical and legal questions regarding parental rights, the minor’s capacity to make informed decisions, and the state’s interest in preserving life.
Read the original article here
Jehovah’s Witnesses have recently announced a significant shift in their long-standing policy regarding blood transfusions, a change that has generated considerable discussion and reaction. For decades, the organization has prohibited members from accepting blood transfusions, a stance rooted in their interpretation of certain biblical passages. This new adjustment, however, allows for members to have their own blood drawn and stored for potential re-infusion during medical procedures.
This evolving understanding of medical practices by church leadership is being framed as a reflection of evolving medical ethics and a greater concern for member welfare. This move, while presented as a positive development, has been met with a range of emotions, from relief to deep-seated criticism, particularly from those who have witnessed or experienced the direct consequences of the previous strict prohibition.
The practical implications of this updated policy are considerable, especially for medical professionals. Anesthesiologists, for instance, note that this new allowance is primarily feasible for planned surgeries. The logistical challenges are substantial; it requires hospitals that can accommodate the preoperative withdrawal of blood and its subsequent storage specifically for the patient. This is no small feat, particularly for smaller medical facilities. Furthermore, the core restriction remains: members are still not permitted to receive blood from other individuals.
Many observers have pointed out the timing of this change, suggesting it comes after a long period where the absolute prohibition on blood transfusions led to tragic outcomes. There’s a pervasive sentiment that this course correction, however it’s being spun by leadership, is a direct response to the negative publicity and legal entanglements that have arisen from preventable deaths. The idea that religious doctrine is evolving to align with medical reality is seen as positive, but the delay in making such a life-saving adjustment is a significant point of contention for many.
A particularly sensitive aspect of this issue is the impact on children. The previous doctrine meant that children, unable to make their own informed decisions, were subject to the same strict prohibition as adults. Many have expressed outrage and deep sadness that children have died because of this rule, and the current change raises questions about the many lives that might have been saved if this policy had been enacted sooner. The lack of an apology from the leadership for past deaths is also a recurring theme in discussions surrounding this policy shift.
The concept of storing one’s own blood, known as autologous transfusion, has been a common medical practice for scheduled surgeries for some time. It involves collecting and testing a patient’s blood units ahead of a planned procedure. While this is a recognized medical procedure, the complexities and limitations, especially in emergency situations, are significant. If a traumatic injury occurs and a patient is bleeding profusely, having not pre-stored blood would render this new policy useless in that immediate crisis.
The medical intricacies of blood transfusions themselves are often overlooked. The rigorous laboratory work involved in ensuring the safety and compatibility of every unit, even in emergency situations, is a testament to modern medicine’s advancements. Each transfusion carries inherent risks, such as sensitization to blood group antigens, which is why cross-matching results have expiration dates. Blood types are generally stable, but antibody screening can change, requiring careful selection of compatible units, especially for patients needing frequent transfusions.
For those who have left the Jehovah’s Witnesses faith, this policy change often brings back painful memories. They recall instances of family members, friends, and even children who died or suffered immensely due to the strict “No Blood” doctrine. The sense of betrayal and anger is palpable, with many feeling that the organization’s leadership has caused irreparable harm by holding onto an interpretation of scripture that has proven to be so devastating.
The idea that this change is a mere “about-turn” without apology, particularly after so many individuals have made the ultimate sacrifice based on the prior doctrine, is deeply unsettling to many. Some speculate that the impetus for this change may have come from within the leadership itself, perhaps due to a high-ranking member facing a critical medical need. This suspicion, whether founded or not, highlights a broader distrust of the organization’s motives.
The implications for religious adherence are also being considered. Some suggest that as membership numbers dwindle, organizations may become more pragmatic, adapting doctrines to ensure the survival of existing members. This, in turn, raises questions about the nature of faith when it appears to be shaped by external pressures and practical necessities rather than purely theological conviction. The comparison is drawn to how other religions have evolved and split over time, suggesting that this shift might be a sign of a similar process for Jehovah’s Witnesses.
Ultimately, while the easing of rules on blood transfusions may be viewed as a step forward by some, for many it is a stark reminder of the profound human cost of rigid religious dogma. The past deaths, the lingering trauma, and the fundamental questions about the leadership’s accountability continue to dominate the conversation surrounding this significant policy revision.