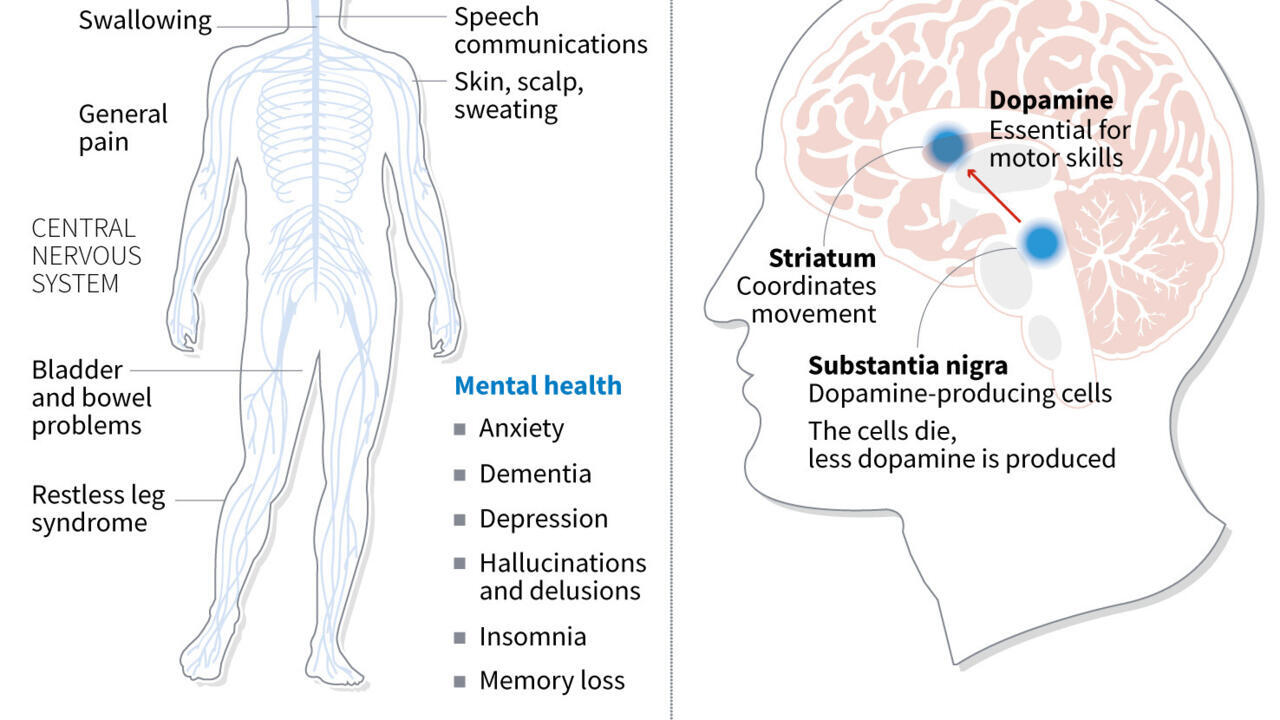
Japan’s health ministry has approved two groundbreaking stem cell-based therapies, Amchepry for Parkinson’s disease and ReHeart for heart regeneration, marking a significant milestone as the world’s first commercially available iPS cell medical products. These treatments, developed by Sumitomo Pharma and Cuorips respectively, hold the potential to revolutionize patient care, with Amchepry showing promise in symptom improvement and safety for Parkinson’s patients in clinical trials. The approval, granted under a system designed for expedited patient access, signifies a new era in regenerative medicine, offering hope to millions worldwide.
Read the original article here
Japan has taken a truly remarkable step forward, becoming the first country to approve a stem-cell treatment for Parkinson’s disease. This significant development comes from Sumitomo Pharma, which received the green light for its treatment named Amchepry. What makes Amchepry so revolutionary is its method of transplanting stem cells directly into a patient’s brain, offering a glimmer of hope for those battling this debilitating neurological condition. It’s understandable why this news would resonate deeply, especially for those who have witnessed firsthand the impact of Parkinson’s on loved ones.
This groundbreaking approval is part of a broader wave of regenerative medicine advancements in Japan. Alongside Amchepry, the country’s health ministry has also given the nod to ReHeart, a treatment developed by the medical startup Cuorips. ReHeart utilizes heart muscle sheets designed to encourage the formation of new blood vessels and restore heart function, highlighting Japan’s commitment to pioneering new therapies for a range of health issues.
The concept behind Amchepry isn’t entirely new, echoing earlier research from the late 1990s and early 2000s. Back then, fetal nigral neurons were transplanted into the brains of Parkinson’s patients. While that approach showed promise, it ultimately faced challenges with inconsistent results and questions surrounding the long-term survival of the transplanted cells, leading to its discontinuation. Amchepry builds upon this foundational idea, but crucially, it uses induced pluripotent stem cell (iPSC) neurons instead of fetal neurons. This distinction is significant, and it will be fascinating to see if this new approach effectively addresses the past concerns associated with fetal grafts.
The potential implications of this approval are vast. For the four patients who have already undergone the treatment and shown improvements over two years, the results are incredibly encouraging. While the specific details of these improvements are not yet widely disseminated, the very fact that such progress has been observed is cause for celebration. The speed at which Japan has moved on this is also noteworthy, especially when considering the slow pace of progress in some other parts of the world.
Japan’s proactive approach to scientific advancement, particularly in areas like regenerative medicine, is particularly striking given its demographic realities. With an aging population and a declining birth rate, the nation’s focus on innovation in health and well-being can be seen not just as a scientific pursuit, but as a matter of cultural survival and ensuring a higher quality of life for its citizens as they age. This makes their investment in cutting-edge medical technologies all the more understandable and strategic.
The question of whether other countries will follow suit quickly is on many minds. There’s a palpable frustration among some that other nations haven’t embraced stem cell treatments more readily. This has led to speculation about the reasons behind this hesitancy, with some suggesting that vested interests within larger pharmaceutical companies might be at play, potentially seeking to protect existing markets or slow down the adoption of these disruptive technologies.
The approval of Amchepry also brings up the practicalities for individuals seeking treatment, such as the potential for medical tourism. Japan is already recognized as a significant destination for medical tourism, and treatments like this could further solidify its reputation. However, the cost of such advanced therapies for international patients is expected to be substantial, raising concerns about accessibility and equity. It’s a reminder that while scientific progress is essential, ensuring broad access to these life-changing treatments remains a significant challenge.
A key point of discussion surrounding stem cell therapies often involves ethical considerations, particularly concerning the sourcing of the cells. While Amchepry utilizes iPSCs, which are derived from adult cells and reprogrammed, earlier research often involved embryonic or fetal stem cells, which have been the subject of considerable ethical debate and political opposition in some regions. Japan’s regulatory framework, which has been rewritten to specifically fast-track regenerative medicine, allows for conditional approval much earlier than many other countries, including the United States. This accelerated pathway is what has enabled Amchepry to reach patients so relatively quickly.
Looking ahead, the impact of this approval could be profound, not just for Parkinson’s patients but potentially for other neurodegenerative diseases as well. The hope is that this successful application of stem cell technology will pave the way for similar breakthroughs in treating conditions like dementia, Alzheimer’s, and other ailments that affect cognitive function and quality of life. While dementia itself, characterized by permanent protein damage, may not be directly reversible, treatments that can slow or halt the progression of neurodegenerative processes are invaluable.
Ultimately, Japan’s pioneering move in approving Amchepry represents a significant milestone in the fight against Parkinson’s disease. It underscores the country’s dedication to scientific innovation and offers a powerful beacon of hope for patients worldwide. The success of this treatment will undoubtedly be closely watched, and it may very well usher in a new era of regenerative medicine, revolutionizing how we approach and treat some of the most challenging diseases facing humanity.