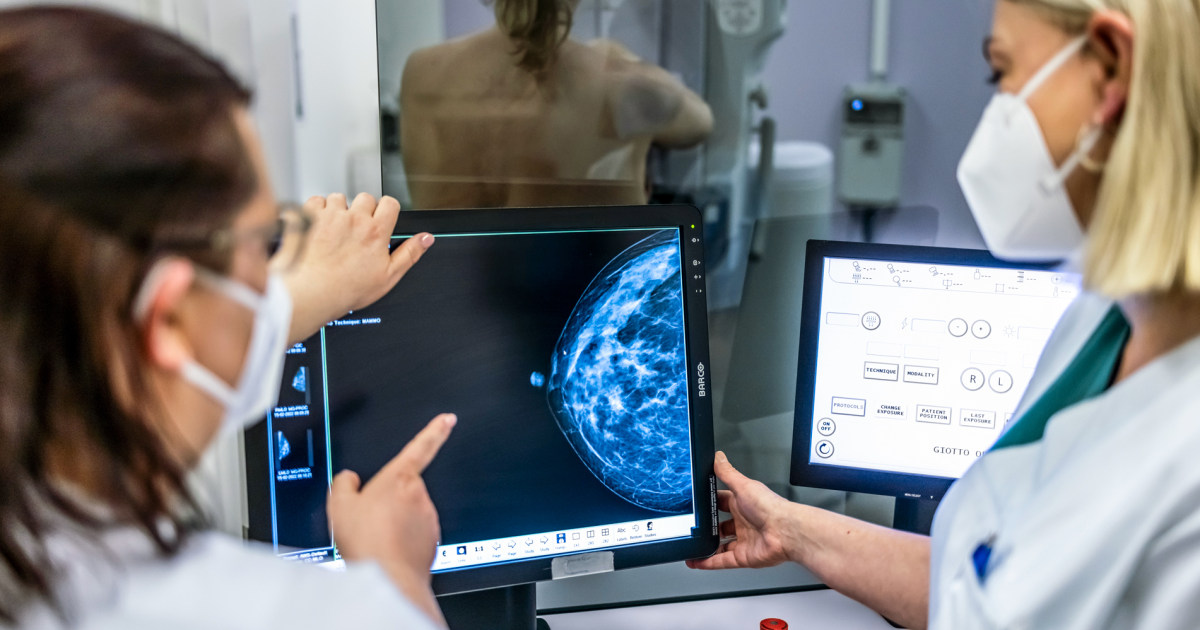
The U.S. Preventive Services Task Force (USPSTF), an independent panel that guides preventive care coverage for over 150 million Americans, has not convened for a formal voting meeting in nearly a year. This delay, attributed to factors including government shutdowns and a reduced membership, raises concerns about the timely updating of crucial health recommendations. The task force’s decisions, which determine which services insurers must cover at no cost to patients under the Affordable Care Act, are considered vital by clinicians for evidence-based medical practice. Uncertainty surrounding the task force’s future, particularly in light of potential political influence on other federal advisory groups, has led to apprehension about the potential politicization of scientific guidance.
Read the original article here
It’s quite concerning to learn that the federal panel responsible for crucial cancer screening recommendations hasn’t convened in nearly a year. This delay, especially given the vital role this group plays in guiding preventive healthcare, raises some serious questions about priorities.
The task force itself is comprised of dedicated volunteer experts from a wide range of primary care disciplines, including internal medicine, pediatrics, family medicine, obstetrics and gynecology, nursing, and psychology. Beyond their clinical expertise, these individuals also bring valuable methodological experience in areas like epidemiology, biostatistics, health services research, decision sciences, and health economics, all of which are essential for developing sound, evidence-based recommendations.
This isn’t a new or ad-hoc group; the task force has been a fixture in preventive healthcare since 1984. Their work is designed to review the latest scientific evidence and translate it into actionable recommendations for screening and other preventive measures that can save lives and improve health outcomes.
A particularly important aspect of the task force’s work is that their recommendations, specifically those earning an “A” or “B” grade, have significant implications for patient access. By law, these high-tier recommendations, which include widely recognized screenings like those for colorectal and breast cancer, are mandated to be covered by health insurers without any out-of-pocket costs for patients. This ensures that cost is not a barrier to essential preventive care.
The fact that this panel, which has historically met regularly to update its guidance, has gone almost a year without a meeting suggests a potential lapse in oversight or a shifting of focus away from public health initiatives. This is especially troubling when considering the potential for advancements and new evidence to emerge in the field of cancer screening, which could lead to more effective and timely detection methods.
One can’t help but wonder if broader economic considerations are inadvertently influencing the pace of these critical health recommendations. The notion that people dying before retirement might be seen as a service to the country from a social security cost perspective is a grim thought, and it raises concerns about whether the well-being of the populace is being prioritized.
It’s important to differentiate this federal panel from independent organizations like the National Comprehensive Cancer Network (NCCN). The NCCN typically meets twice a year to update its practice guidelines and operates independently of government. The updates provided by such independent bodies are vital for ensuring that patients continue to receive the most current and effective treatment and screening advice.
There’s a prevailing sentiment that when certain administrations are involved in healthcare policy, their actions can sometimes lead to negative outcomes. The idea of working harder and dying faster, or a general distrust of recommendations from a particular administration, speaks to anxieties that public health might be taking a backseat.
The overarching concern seems to be the potential for a disconnect between economic interests and public health goals. The idea that letting people die off might be seen as beneficial for the economy or that it could interfere with certain profit margins, particularly within the “cancer biz” where there’s significant financial investment, is a deeply unsettling prospect.
The absence of meetings from this critical federal body raises questions about a potential prioritization of other agendas, perhaps those that are perceived as more economically advantageous, over proactive and life-saving preventive care. This situation highlights the importance of consistent and timely review of health recommendations to ensure that the public benefits from the latest scientific understanding in the fight against diseases like cancer.